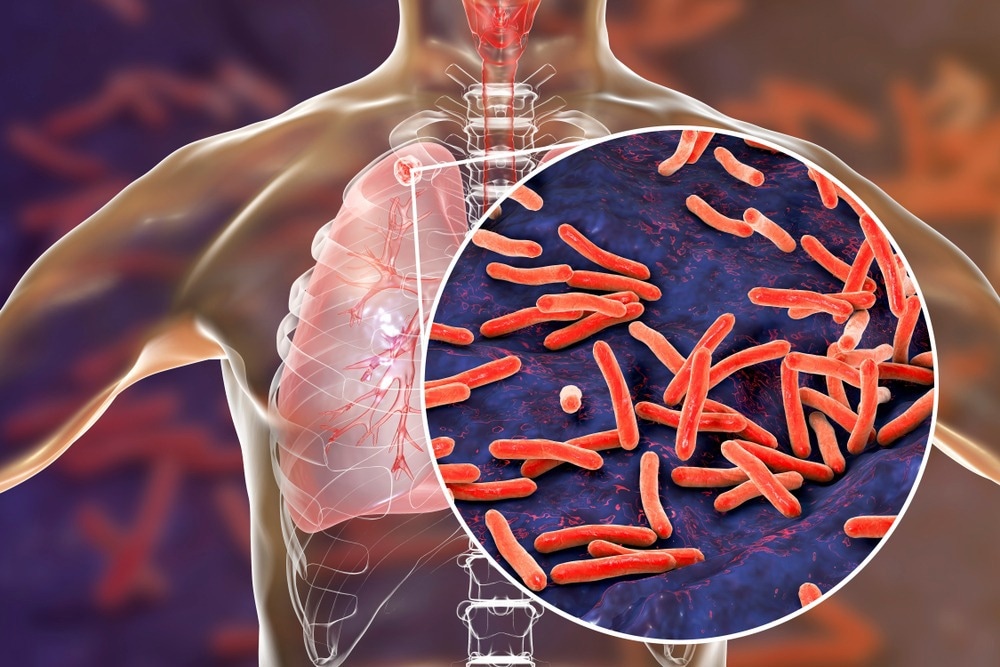
A recent study published in PLOS Pathogens discussed coinfections in the lungs and how viral infections create a favorable environment for bacteria and fungi.

Background
Secondary bacterial infections can influence the morbidity/mortality of individuals with respiratory viral infections; however, bacterial infections are not the sole threat to them. That is, the incidence of patients with respiratory viral infections contracting secondary fungal infections, especially involving Aspergillus fumigatus, has increased over the past decade.
Although secondary fungal infections are relatively less frequent, they are associated with higher mortality. In the present study, researchers discussed how host antiviral responses in the lungs could create an environment permissive for bacterial and fungal infections.
Aftershocks of viral infections
The physiologic outcomes of respiratory viral infections include altered respiratory function, epithelial damage, and delayed repair, while the immunologic effects are a little more complicated. A recent transcriptional analysis of samples from patients with influenza-associated pulmonary aspergillosis (IAPA) suggested disruptions in anti-fungal immunity, affecting epithelial barrier integrity, phagocytosis ability, and the capacity to destroy hyphae/conidia.
Physiologic aspects
Aspergillus spp. differ from bacterial species involved in secondary infections in being saprophytic. The growth and survival of molds depend on the decay of the surrounding environment. Antiviral responses contribute to physical damage within the lungs. This decomposed-like state likely contributes to establishing lung infection with Aspergillus spp. following viral infections, as observed by fungal growth near damaged epithelium in IAPA and coronavirus disease 2019 (COVID-19)-associated pulmonary aspergillosis (CAPA).
Specifically, nutrient acquisition (by the fungal pathogen) would become more accessible due to the death of cells and the vasculature/epithelial leak, increasing the availability of macromolecules and essential nutrients. Besides, adaptability to changing environments is vital to establishing a fungal infection. Lung inflammation and damage decrease oxygen availability. Generally, Aspergillus spp., specifically A. fumigatus, show quick and efficient adaptation to low-oxygen conditions, which helps resist anti-fungal drugs and immune responses.
Immunologic aspects
During infection, Aspergillus spp. go through three stages of growth – resting/dormant conidia, swollen conidia, and hyphae forming a biofilm. The host immune system employs different tools for each stage, and preventing hyphal growth remains the ultimate goal, which could be accomplished by conidial destruction. Alveolar macrophages are the first line of defense that ingest and kill conidia in the airways.
A. fumigatus susceptibility increases when alveolar macrophages become impaired. Neutrophils and monocytes are also critical for eliminating conidia. Evidence suggests that disrupted epithelia, reduced alveolar macrophages, and dampened inflammatory responses in secondary bacterial infections influence the activation/recruitment of these immune cells, which will likely hold for secondary fungal infections.
Reactive oxygen species (ROS)-dependent or independent mechanisms are critical for resistance to A. fumigatus, which are impaired during viral infections. Neutrophil extracellular traps (NETs) also act as anti-fungal mechanisms to control hyphal growth. However, excess NET formation from post-viral infection neutrophils might contribute to the damage instead of clearing the fungal pathogen, as observed in lung injury models.
Previously, the current study’s authors reported that prior viral infections impact anti-fungal ROS-independent pathways, particularly phagolysosome maturation. Further, reduced levels of pattern recognition receptors (PRRs) post-viral infection have been associated with poor outcomes during secondary bacterial infections. However, while the PRRs are implicated in anti-fungal immunity, whether they have a direct role in IAPA remains unclear.
C-type lectin receptors (CLRs) have a critical role in protecting against fungal infections. CLRs help distinguish conserved pathogen-associated molecular patterns (PAMPs) in fungal cell walls and elicit specific immune responses. Reduced expression of an essential CLR was observed in an ex vivo influenza infection model of alveolar macrophages. However, less is known about CLR signaling in influenza and IAPA.
Concluding remarks
Most classical risk factors associated with a higher Aspergillosis risk are not common among patients with IAPA or CAPA, which could result in lower testing rates, misdiagnosis, and delays in treatment. This could be detrimental for patients as treatment delays may allow Aspergillus spp. to develop into a more robust and resistant biofilm. Above all, there is a need to deepen the understanding and increase the knowledge base of host-fungal interactions following viral infections to develop specific therapies.